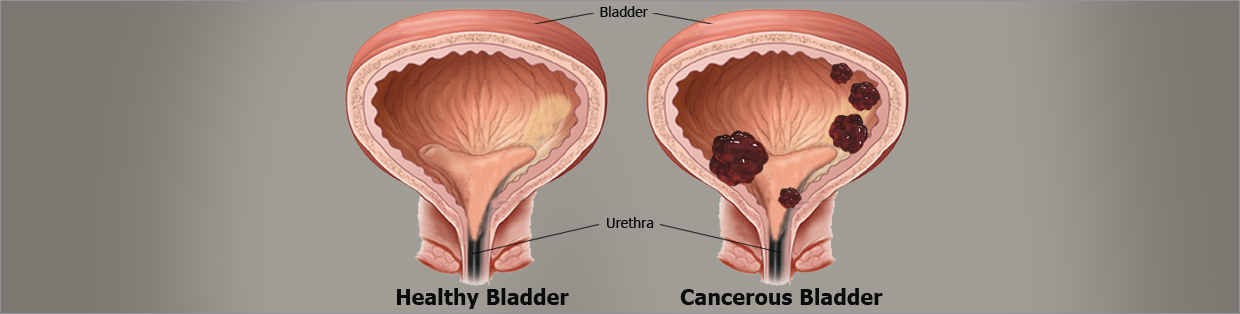
Know about Urinary Bladder Cancer
Overview
Urination (micturition) involves physiological processes within the urinary tract and the brain. The slight need to urinate is sensed when urine volume reaches about one-half of the bladder's capacity. The brain suppresses this need until a person initiates urination.
Neurons in the brain and in smooth muscle of the bladder govern the detrusor muscle (layered smooth muscle that surrounds the bladder); it is not controlled voluntarily. The nervous system stimulates the detrusor muscle to contract into a funnel shape and expel urine, once a person initiates urination. Pressure in the bladder increases and the detrusor remains contracted until the bladder empties. Once empty, pressure falls and the bladder relaxes and resumes its normal shape. If bladder pressure remains high while the bladder is filling, the bladder contracts erratically. Normally, the detrusor muscle contracts and relaxes according to the volume of urine in the bladder and the initiation of urination. In people with an overactive bladder, the detrusor muscle contracts spastically, sometimes without a known cause, which results in sustained, high bladder pressure. People with the condition typically experience the urgent need to urinate at inconvenient times and may lose control before reaching a toilet. Overactive bladder interferes with work, daily routine, and intimacy; causes embarrassment; and may diminish self-esteem and quality of life.
Incidence and Prevalence
Overactive bladder affects men and women equally. Approximately 20 million people in the United States suffer from the condition. Though it is not necessarily a result of aging, it most often affects older people.
Causes
Malfunctioning detrusor muscle in the smooth muscle of the bladder causes overactive bladder. Identifiable underlying causes include the following:
- Abdominal or pelvic trauma or surgery resulting in nerve damage
- Bladder stones
- Drug side effects
- Neurological disease (e.g., multiple sclerosis, Parkinson's disease, stroke, spinal cord lesions)
Other conditions can produce symptoms similar to those experienced with overactive bladder, the most common of which is urinary tract infection (UTI) in women.
Signs and Symptoms
Three symptoms are associated with an overactive bladder:
- Frequency (frequent urination)
- Urgency (urgent need to urinate)
- Urge incontinence (strong need to urinate followed by leaking or involuntary and complete voiding)
Treatment
Treatment may include one or more of the following:
- Bladder retraining
- Medication
- Sacral Nerve Stimulation
- Surgery
Medications such as oxybutynin chloride (Tropan XL®) and tolterodine (Detrusitol®, Terol®) are once-a-day oral medications for overactive bladder that can improve symptoms in as little as 2 weeks. These drugs (antimuscarinics) affect the central nervous system and muscarinic receptors in smooth muscle that control detrusor muscle. They relax the smooth muscle of the bladder, which reduces detrusor contraction and subsequent wetting accidents. In a recent study, participants taking Tropan XL had 90% fewer accidents, used fewer protective pads, and experienced 24-hour relief from urgency and loss of control.
Side effects, including dry mouth, constipation, headache, blurred vision, hypertension, drowsiness, and urinary retention occur in approximately 50% of those who use the drugs. People with certain types of kidney, liver, stomach, and urinary problems, or glaucoma are advised not to take Tropan XL®. Although there is no evidence that Tropan XL causes birth defects, pregnant women should not take it without consulting a physician.
Sacral Nerve Stimulation
Interstime Therapy for Urinary Control is a reversible treatment for people with urge incontinence caused by overactive bladder who do not respond to behavioral treatments or medication. Using an implanted neurostimulation system, InterStim Therapy sends mild electrical pulses to the sacral nerve, a nerve near the tailbone in the lower back that influences bladder control muscles. Stimulation of this nerve may relieve the symptoms related to urge incontinence.
Prior to implantation, the effectiveness of the therapy is tested with an external device. For a period of 3 to 5 days, the patient records voiding patterns with the stimulation. The test is done on an outpatient basis and the diary is compared to patterns identified previously to determine if treatment is effective.
Candidates for InterStim Therapy first undergo a test stimulation to determine how responsive they are to the therapy. The test provides information to determine if the device is a viable treatment option, such as the effect of sacral nerve stimulation on symptoms and how the patient experiences the stimulation.
If the test is successful, a patient may receive an implanted InterStim System. The procedure requires general anesthesia. A lead (a special wire with electrical contacts) is placed near the sacral nerve and is passed under the skin to a neurostimulator, which is about the size of a stopwatch. The neurostimulator is placed under the skin in the upper buttock.
Adjustments to the stimulation can be made at the doctor's office, with a programming device that sends a radio signal through the skin to the neurostimulator. An additional programmer is given to the patient to allow further adjustments to the level of stimulation, and the system can be turned off at any time.
Possible adverse effects include the following:
- Change in bowel function
- Infection
- Lead movement
- Pain at implant sites
- Unpleasant stimulation or sensation
Surgical augmentation of the bladder is reserved for people who do not benefit from bladder retraining or medication. Those who cannot take medication due to medical conditions or intolerance may find incontinence management devices helpful.